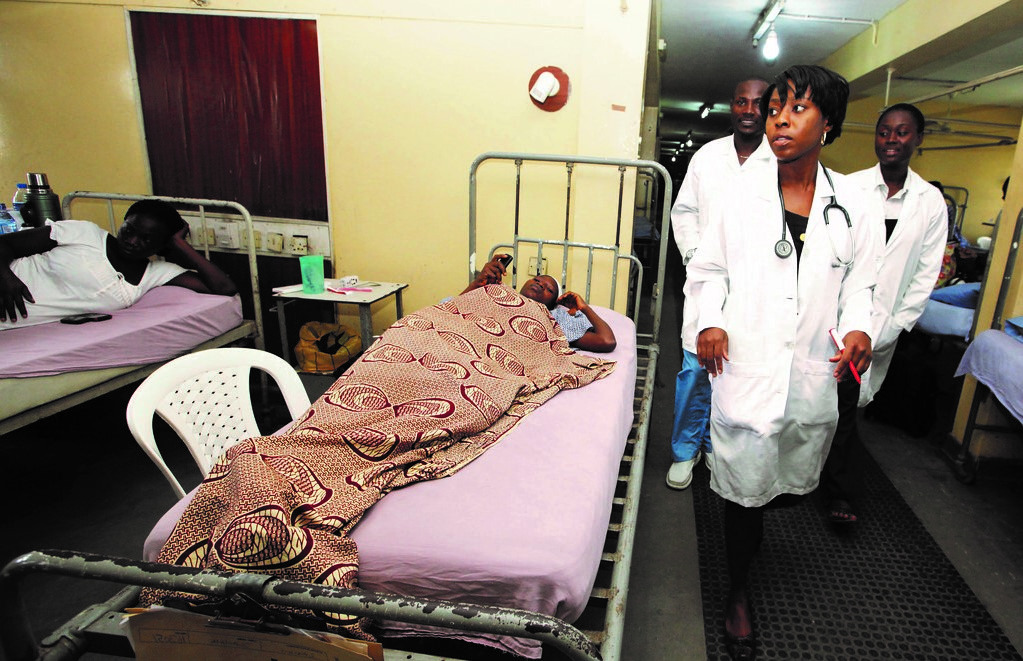
SHOPS Plus, USAID’s flagship initiative for private-sector health care, implemented a gender-supportive supervision activity in Nigeria. Their goal? Improve performance, retention, and gender equity for voluntary family planning providers.
Nigeria, Africa’s most populous nation, certainly has a big stake in the reproductive health arena. The country has a population of 200 million people and a birth rate of 2.6% per year, according to 2019 World Bank figures. Access to quality and voluntary family planning care is an essential element in its development agenda, and family planning providers are right at the center.
Effective service provision is key to delivering timely and affordable family planning care. Yet the quality and swiftness with which these services are provided in Nigeria face numerous and diverse barriers, including those related to gender.
Voluntary Family Planning Providers Face Gender-Related Workplace Challenges
According to SHOPS Plus, the USAID-funded flagship initiative for private sector health-care led by Abt Associates in Nigeria, voluntary family planning providers can experience significant gender-related biases and barriers to successfully delivering family planning care to their clients. Female health workers sometimes face safety concerns in the workplace; often the bias exists that male providers are more competent; and sometimes health workers face occupational segregation (for example, men are often excluded from being nurses).
These scenarios in Nigeria form part of the global outlook. Gender equity is a subject of deserved attention in the global health-care workforce. The World Health Organization (WHO) stated last year that while gender has a significant impact on workplace experiences and interactions in health care settings, global efforts to address gender barriers and inequalities for health-care providers in the workplace are limited. While the public health frontline workforce is disproportionately female, we do not see many women in positions of public health leadership. WHO statistics show that women comprise 70% of the health-care workforce globally, yet hold only 25% of senior positions.
In Africa, the gender gap in the health-care workforce is significant. 72% of physicians are male and 28% are female, while 65% of nurses are female and 35% are male. Overt gender bias and discrimination, lack of mentorship opportunities, and challenges related to managing family responsibilities and meeting promotion criteria are among the contributing factors. These factors, however, may vary from one country to another.
Gender-Transformative Supportive Supervision Addresses Gender Disparities in the Voluntary Family Planning Workforce
Gender-transformative supportive supervision (GTSS) is one model to address the gender disparities we see across the family planning workforce. In Nigeria, SHOPS Plus piloted the GTSS model, applying it to family planning care. Dr. Shipra Srihari, a researcher at SHOPS Plus, argues that voluntary family planning providers in both private and public health facilities can face multiple barriers in the workplace related to their gender, several of which could be addressed, in part, by their supervisors through supportive supervision. Traditionally, she adds, human resource management interventions, including supportive supervision, have generally been implemented without attention to how gender norms and power dynamics might affect experiences in the workplace or the relationship between supervisors and actual service providers.
Paulina Akanet, the family planning lead for the SHOPS Plus program in Nigeria, explains that gender-transformative supportive supervision aims to improve provider performance, retention, and gender equity in the workplace. The model integrates gender into standard supportive supervision training for supervisors and introduces tools for supervisors that promote discussions around gender. In Nigeria, the training on supportive supervision included a gender module that helped supervisors understand and challenge their own gender biases, and trained them on how to have constructive conversations with their supervisees about gender barriers in the workplace.
“The ‘theory of change’ was that once trained, supervisors would provide gender-transformative supervision to the providers they supervise,” explains Dr. Srihari. “In other words, in their supervision of family planning providers, they would conduct supervision with reduced gender bias, initiate constructive conversations about gender in the workplace with the health-care providers they visit and supervise, and work with providers to address any emerging gender-related issues in the workplace.”

Using GTSS to Improve Communication between Staff and Supervisors
Nankang Andrew, a midwife at Plateau State Hospital, a public health facility in Plateau State, is one of the family planning providers trained by SHOPS Plus; her supervisor was trained on GTSS. She agrees that training improved communication and interactions with her supervisor—so much so, her supervisor checks to see how he can support her in balancing work and family responsibilities. Dr. Srihari shares that their program is transforming supportive supervision by moving away from the conventional supervisory checklists that primarily focus on clinical skills to clinical skills supervision integrated with prompts to discuss gender-related barriers in the workplace.
Dr. Srihari also emphasizes that since GTSS is a new model, their goal was to understand and learn from the implementation process. “We were focused on understanding how the model was received by providers and supervisors, and whether or not their experience suggests movement towards better family planning provider outcomes,” she explains.
Achieving gender-transformative supervision and gender equity in the workplace, however, is a gradual process. It requires multiple coordinated strategies that promote professional development and women’s leadership while addressing social norms and perceptions of gender. Assessment of GTSS outcomes revealed that while many providers and supervisors generally felt comfortable discussing issues around gender in the workplace during supervision sessions, and the issues raised indeed resonated with many of them, a significant number had difficulty grasping the reality of gender dynamics they relate to providers. Dr. Srihari attributes this to a number of factors, including either the complexity of gender concepts and barriers in the workplace and appreciation of the subject, or the implicit nature of gender roles in society.
Some family planning supervisors and providers reported difficulty distinguishing providers’ gender workplace issues, such as the bias about male providers being perceived as more competent than female providers, from issues related to clients’ gender, which are related to biases the client may face due to their own gender. While both are important issues, and the SHOPS Plus program does address issues related to client gender in their family planning training for providers, Dr. Srihari stresses that the GTSS intervention particularly focused on addressing gender barriers that the provider, not the client, faces in their workplace.
Documenting Nigeria’s Experience with Gender-Transformative Supportive Supervision
In the coming months, SHOPS Plus will be publishing a brief on GTSS in Nigeria to encourage more learning and sharing of best practices. In general, Nigeria’s experience with piloting GTSS demonstrates that quality supportive supervision that is interactive and collaborative can lead to positive outcomes among family planning providers. Accompanied by structural and policy changes in health-care work settings, gender-transformative supportive supervision could contribute to both improved quality of care for clients, and ultimately to a more equitable workplace for providers in both the public and private health-care sectors.