Cervical Cancer Prevention: A Life-Course Approach to SRH
Q&A Conversation with TogetHER for Health and Population Services International
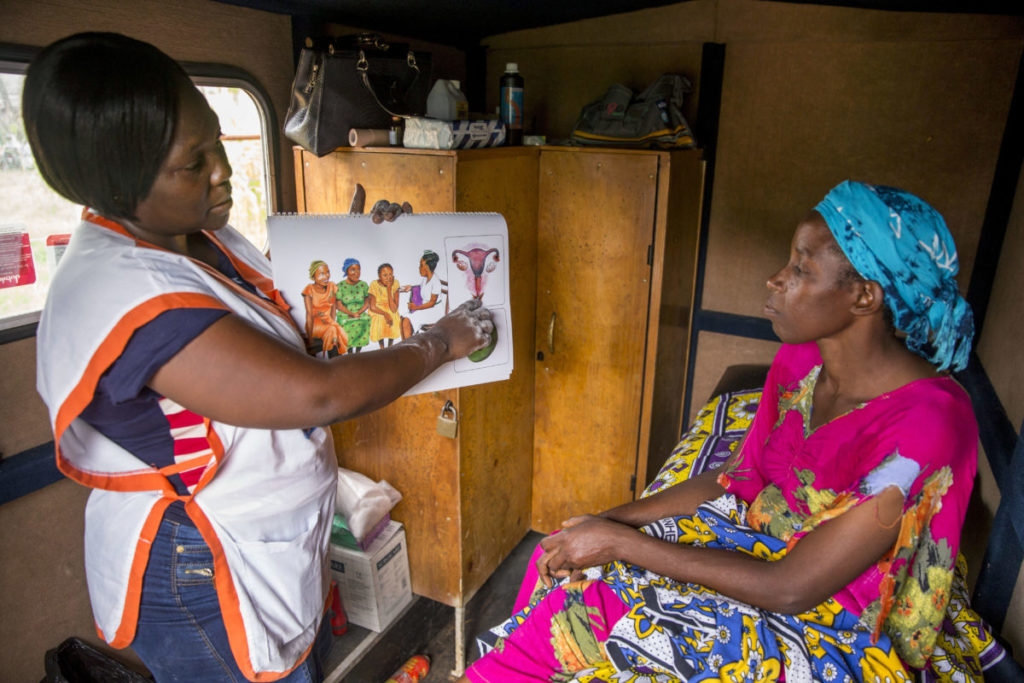
Recently, Brittany Goetsch, a Program Officer on the Knowledge SUCCESS project, chatted with TogetHER for Health’s Executive Director, Dr. Heather White, and Population Services International’s (PSI’s) Global Medical Director, Dr. Eva Lathrop, on the integration of cervical cancer into broader SRH programming and what cervical cancer can teach us about a life course approach to SRH.
In addition, while in Mozambique recently, Dr. Eva Lathrop spoke with the nurse coordinator for PSI’s PEER Project, Guilhermina Tivir.
Learn more about cervical cancer and SRH in the companion piece, A Life-Course Approach to Reproductive Health.
Introductions
Brittany Goetsch: Can you tell me a little bit more about your current role and what you do with TogetHER for Health and PSI?
 Heather White, TogetHER for Health: TogetHER for Health is largely an advocacy organization. We work to increase visibility and funding for cervical cancer prevention both globally and in the U.S. TogetHER works across three pillars: 1) we conduct advocacy to global funders like the U.S. government to include funding for global cervical cancer prevention; 2) we work alongside implementing organizations to understand and identify best practices in prevention programs; and 3) we conduct communication campaigns to share the stories of women, families, and communities affected by this disease. Along with women and their families, frontline health care providers are an important population for us to interact and engage with.
Heather White, TogetHER for Health: TogetHER for Health is largely an advocacy organization. We work to increase visibility and funding for cervical cancer prevention both globally and in the U.S. TogetHER works across three pillars: 1) we conduct advocacy to global funders like the U.S. government to include funding for global cervical cancer prevention; 2) we work alongside implementing organizations to understand and identify best practices in prevention programs; and 3) we conduct communication campaigns to share the stories of women, families, and communities affected by this disease. Along with women and their families, frontline health care providers are an important population for us to interact and engage with.
 Eva Lathrop, PSI: In my role as the Global Medical Director, I support all of our programming and technical work in SRH, which includes cervical cancer. Right now, PSI has SRH programs in over 20 countries, and of these, we’re working in 8-9 on cervical cancer prevention and treatment programs using new technologies or existing technologies like visual inspection. Most of our cervical cancer [programs] are integrated into existing clinical services. Historically, we’ve also had work in HPV vaccination campaigns in Trinidad & Tobago.
Eva Lathrop, PSI: In my role as the Global Medical Director, I support all of our programming and technical work in SRH, which includes cervical cancer. Right now, PSI has SRH programs in over 20 countries, and of these, we’re working in 8-9 on cervical cancer prevention and treatment programs using new technologies or existing technologies like visual inspection. Most of our cervical cancer [programs] are integrated into existing clinical services. Historically, we’ve also had work in HPV vaccination campaigns in Trinidad & Tobago.
Brittany: How did you become interested in this work?
Eva: I’m an OBGYN by training, so cervical cancer work across the spectrum and across the life course has always been a part of my clinical work and training. Somehow we are still seeing women across the globe including in the United States, dying of cervical cancer. This is such a reachable goal—elimination [of cervical cancer]. The vast majority of cervical cancer cases and deaths can be prevented by many levels of prevention—one of them is the vaccine, and through early screening, and screening at regular intervals. To me, this has always been a frustrating area of interest, but I think we’re getting there globally. I think the only way to do it is through a consortium of partners and by prioritizing this work along with the other SRH work we’re doing.
Heather: I’m a public health practitioner by training. I first learned of cervical cancer as a public health issue in 2006 when PEPFAR first initiated funding to integrate cervical screening for women living with HIV for cervical cancer into PEPFAR country programs. As part of my doctoral program, I conducted a small study at local health clinics in Lusaka, Zambia to better understand social and cultural aspects of this disease among Zambian women: were they familiar with this disease; was cervical cancer discussed among women; was screening a priority, and why or not. When women came for screening, I wanted to understand their perceptions and acceptability of the screening process, in order to improve the patient-provider experience. Once I completed my doctoral program, I was hired at PSI as their global technical lead in cervical cancer prevention, and supported the design, implementation, and evaluation of screening and pre-cancer treatment programs across multiple countries across PSI’s global portfolio of SRHR programs.
Want to know more?
Listen to Eva and Heather discuss what made them interested in this work.
Main Challenges
Brittany: What are some of the main challenges to cervical cancer prevention and treatment that confront the work that PSI and TogetHER for Health are doing? Can you talk a little bit more about why it’s called “preventable cancer” and how this informs program priorities?
Heather: As Eva alluded to, this is the one cancer that we know enough from a scientific point of view to know what causes it, how to prevent [it], and how to treat it. The vast majority of cervical cancers can be prevented with three complementary interventions: HPV vaccination, ideally between 9–14 years of age; cervical screening among adult women; and timely follow-up and treatment for any women with cervical abnormalities. Those three interventions are straightforward, and yet logistically and operationally challenging to put in place around the globe! Nevertheless, that is the challenge ahead of us: to make headway towards global elimination of HPV and cervical cancer.
Globally, 9 out of 10 cases of cervical cancer occur in lower- and middle-income countries. This is absolutely a disease of poverty and of inequity. High disease burden is a result of a lack of organized screening programs, and it can be very difficult for women and girls to access these life-saving preventive services in countries with the highest disease burden.
Eva: Barriers to this primary prevention piece include supply chain, cost, and the logistical barriers of having to come back for a second or third vaccine. But it isn’t just that—working outside of the health system and into the education system to try and raise awareness and acceptance of a vaccine that works to prevent a cancer that’s caused by a sexually transmitted virus, and giving the vaccine to kids in elementary school, middle school, and early high school—that’s been a huge challenge socially and culturally across the globe, including and perhaps in particular in the United States. Of all the pieces required to prioritize cervical cancer prevention and make services available, the HPV vaccine part is perhaps the hardest part of those things. When services are available in a health center where a person (such as a woman who is out of school who may already have her family or be in the midst of having her family) is already seeking care for another service, and [the services are] integrated, this is somehow a lower-hanging fruit to build upon and scale than the vaccine pieces. Vaccinating kids is not the most controversial intervention in our global health portfolio, but I would say the HPV vaccine remains controversial.
Want to know more?
Listen to Eva and Heather discuss vaccine campaigns and services.
Barriers women face to cervical cancer prevention: vaccination, screening, and preventive treatment
- Cost of services.
- Lack of awareness: There is a lot of evidence that many women do not know the linkages between HPV and cervical cancer and that screening is an important prevention tool.
- Global HPV vaccine supply shortages. Even if the political will to increase access to the vaccine in a country is present, many countries currently face a significant shortage of vaccines.
- Loss to follow-up with vaccine doses. Two doses have historically been required; however, the recent WHO SAGE recommendations acknowledge that one dose is as effective as two. This change will undoubtedly have a positive impact on HPV vaccine access going forward by removing the practical and logistical barriers of the two-dose regimen.
Applying Lessons from Cervical Cancer to SRH
Brittany: What does cervical cancer teach us about a “life course” approach to SRH?
Eva: I think that cervical cancer across its spectrum is a reminder that there are opportunities for action and intervention beyond cervical cancer and throughout a sexual and reproductive health life, and throughout a life course. We think of care in sexual and reproductive health from the perspective of the years when somebody might be pregnant or having their babies and that there’s nothing before and there’s nothing after, that there’s no need to seek care, no need to prioritize or fund care that might come outside of that. Whether or not somebody is reproducing and having children should in essence, be beside the point. Pregnancy is a great reason for people to seek care; people seek care during pregnancy, deliveries—not always, but often—and [these opportunities] bring people into care. Developing models that are integrated and facilitate adding the other pieces to that care—STI prevention and treatment and detection, cervical cancer screening, and preventive treatment—can all be integrated into those times of high health-seeking behavior.
But then there [are] the rest of our years. We are sexual beings beyond our fertile years! Sexuality does not end when fertility is no longer an issue. Let’s talk about post-fertility years. That doesn’t mean post-sexually active years, post-sexual being years. These are still years [where] people need attention in terms of their health care. Cervical cancer is a good reminder of that. We need to consider reproductive health cancers, we need to consider risk of STI infection, etc. well beyond one’s ability to get pregnant. These reproductive health issues don’t wrap up neatly into years where someone might be [fertile]. And they also don’t necessarily start then. There are all sorts of reasons to support health-seeking and encourage it, and raise awareness around education in the early life course also, around menstrual health, menstrual hygiene, [the] potential risk of sexual encounters or gender-based violence or intimate partner violence, and the potential risk around sexually transmitted infection around those encounters. Across the spectrum, we need to be thinking about the risk of GBV and intimate partner violence throughout the life course.
There are lots and lots of reasons to be paying attention to all these pieces, well beyond somebody’s years where they’re able to get pregnant. For some people, there are no fertile years, but it doesn’t mean that we’re not going to care for all of the other things that happen from a health perspective around somebody’s reproductive life, organs, experiences. We need to take care of people and not make assumptions. I think perhaps there is some gender bias here around women and sexuality and needs beyond pregnancy and reproduction. The providers’ and systems’ perspective is that women don’t need care outside of their ability and the years when they can reproduce—then we have an opportunity to shift this perspective. One of those ways is through prioritizing cervical cancer screening and prevention and then integrating it into other areas of care where women are likely to seek care during different parts of their life course.
Heather: As [Eva] alluded to, and I’ll just maybe emphasize the point, that to me, HPV/cervical cancer prevention is a really great model to look at through a life-course lens because there are multiple opportunities to intervene with safe, effective services across a young woman’s and an adult woman’s life stages. When you look at cervical cancer rates, when women reach 40–49 years, that is often when, because we’re not thinking of childbearing necessarily in those years, women often decide to no longer see their provider because they don’t realize that they still need these services, like cervical screening. Just when a woman is most vulnerable to this disease, she may disappear from the health system. This is why continued education reminders from health care providers are so important. Health communication and education—whether through a campaign, or one-to-one conversations with community health educators, or nurses, midwives, or other providers—is critical, especially for preventive services. Cervical cancer prevention gives us the opportunity—and in fact, the responsibility—to reach a girl or a woman at multiple points across her reproductive life and beyond, and should spur policymakers and program teams to develop holistic strategies that meet her needs at each of these points. This challenges us to be intentional and creative in designing communications, outreach, services, and follow-up with an eye to meet her along a continuum that spans her entire life.
“We know that health is a state of complete wellness. The integration of cervical cancer screening in sexual and reproductive health is a good implementation [practice] because it encompasses all consultations for a woman. To maintain sexual and reproductive health, people need access to accurate information and to safe, effective, affordable, acceptable contraceptive methods of their choice. In terms of programming, it works [well if] women are informed through very clear messages and empowered to protect themselves from sexually transmitted infections—for example, how to use a female condom. When they decide to have children, women should have access to the services that will help them have a safe pregnancy and [a healthy baby]. Services should be of quality and supplies should always be available at health facilities…. [Women] can… resolve all problems in one room, with one provider. I think it’s something we [should] think [about] because it’s amazing.”
Want to know more?
Listen to Guilhermina Tivir, Nurse Coordinator for PSI’S PEER Project, share what she wishes other FP/RH professionals knew about integrating cervical cancer and SRH.
The PEER Project in Mozambique
PSI’s Work
Brittany: Eva, can you tell me a little bit more about PSI’s work in Mozambique and what you were doing there last week?
 Eva: We are part of a fantastic project, Evaluating Innovative Technologies and Approaches to Cervical Cancer in Mozambique (referred to as the PEER Project). This is a clinical trial focused on evaluating new technologies and models of care to address cervical cancer in two provinces in Mozambique…. We are working with a consortium of partners: MD Anderson, PSI, the State University of Mozambique, the Ministry of Health [in Mozambique], Rice University, [Clinton Health Access Initiative], and others. We’re all involved in examining a number of different outcomes; at PSI, as the implementing partner, we’re focused on exploring different models of care that work best for people. That’s largely around looking at integration of cervical cancer screening and prevention into existing family planning models of care in several public facilities. We also have satellites and mobile outreach models. We are learning about what works best for people by talking to people who access and those who provide this care.
Eva: We are part of a fantastic project, Evaluating Innovative Technologies and Approaches to Cervical Cancer in Mozambique (referred to as the PEER Project). This is a clinical trial focused on evaluating new technologies and models of care to address cervical cancer in two provinces in Mozambique…. We are working with a consortium of partners: MD Anderson, PSI, the State University of Mozambique, the Ministry of Health [in Mozambique], Rice University, [Clinton Health Access Initiative], and others. We’re all involved in examining a number of different outcomes; at PSI, as the implementing partner, we’re focused on exploring different models of care that work best for people. That’s largely around looking at integration of cervical cancer screening and prevention into existing family planning models of care in several public facilities. We also have satellites and mobile outreach models. We are learning about what works best for people by talking to people who access and those who provide this care.
There’s a strong qualitative component to our work: we have opportunities to speak with women who seek this care and for providers who are engaged in this care, and for stakeholders and policymakers who are adjacent to—but also critically important to—in terms of what happens next in this care. The second part of this work is figuring out what works to bring people into screening care when [they’re] not otherwise seeking care…. Another piece is examining new technologies for screening and preventative treatment, and the last piece is a costing study to show whether using these cost models is cost-effective.
Want to know more?
Listen to more about the PEER Project in Mozambique.
Listen to Guilhermina explain how she became interested in the PEER Project.
Kizazi Chetu, Kenya
Brittany: Heather, I want to turn to you and ask if you could tell us more about the Kizazi Chetu campaign. Any best practices that have been useful in implementation, and what’s in store for the campaign in 2022?
Heather: Kizazi Chetu means “our generation” in Swahili. We decided to work with a social impact design firm called Scope Impact; they’re based in Helsinki, Finland, but they have a local team in Nairobi. We wanted to put a campaign together that I often say is not your mother’s public health campaign. It’s forward-thinking, it is multi-generational, it’s meant to bring in a younger audience around the elimination agenda … We set our sights on a high-burden cervical cancer country, Kenya. We knew there was a lot of marketing savvy, a lot of reach there too, so we developed the campaign with Scope Impact. We put a strong emphasis on reaching men around this issue, as well as reaching women and young women across generations … What we’re planning to do for this next phase is to bring together stakeholders across counties in Western Kenya to look at how we translate policy that may be on the books at the national or even the county level and move those into practice, specifically thinking about improved technologies. Understanding what representatives across these counties [have] done already with respect to cervical cancer screening and pre-cancer, preventative treatment, what are the barriers and what are the opportunities for some of these newer technologies to become more widespread, what do women understand and what do they think of those technologies … We’ll be working across a 14-county consortium to look at those opportunities and see if we can put some scenarios in which we may be looking at public-private partnerships to do more in increasing access and coverage.
Concluding Thoughts
Hear about Guilhermina’s proudest moment working in the field of cervical cancer and SRH.
Hear what excites Heather and Eva the most about where the cervical cancer and SRH fields are going.
Responses have been slightly edited for clarity and length.





