What is Knowledge Management?
In a hurry? Skip to the quick summary.
Overview
Global health and development work involves a diverse community of individuals and organizations working toward common goals. Groups that are most effective in meeting these goals have systems in place to routinely share critical knowledge, gain immediate access to the latest research, and translate lessons learned into better programs. Knowledge management—the process of collecting and curating knowledge and connecting people to it so they can act effectively—is at the heart of these systems. Knowledge management can improve coordination and enhance meaningful learning, collaboration, and application.
WATCH: An Overview of Knowledge Management and its Key Components
Most knowledge is created, captured, and shared through human interaction—making it essentially a social act.
People must, therefore, be at the core of any knowledge management approach, particularly since so much knowledge is in people’s heads and difficult to transfer to others. People can help cultivate an environment that encourages knowledge exchange and use of knowledge management systems.
Processes, both formal and informal, help us capture, and share knowledge, while technological platforms can expedite knowledge storage, retrieval, and exchange—provided they are used in context.
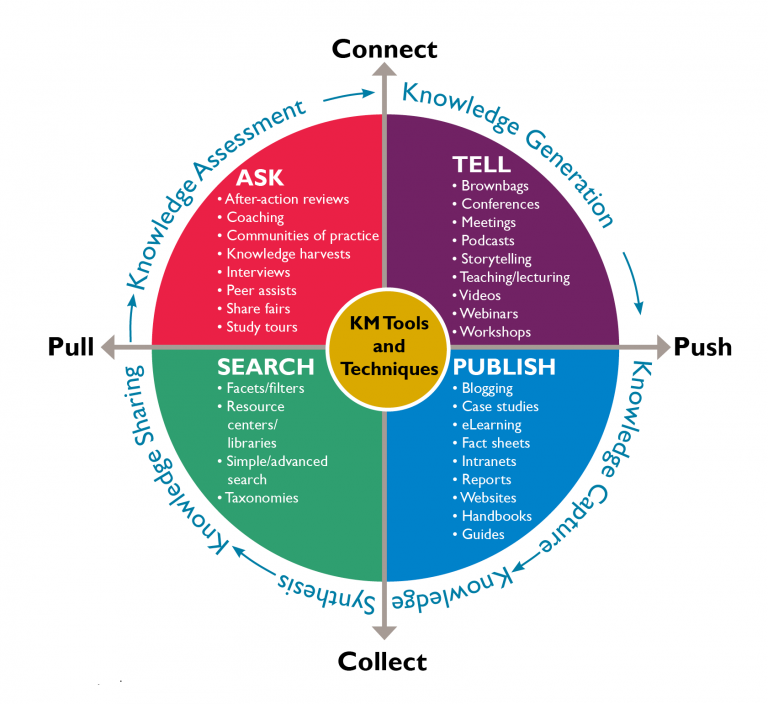
The Knowledge Management Road Map
The Knowledge Management Road Map is a five-step systematic process for generating, collecting, analyzing, synthesizing, and sharing knowledge in global health programs. The steps include:
- Assess needs: Understand the context of the global health program challenge and identify how knowledge management may help solve it.
- Design strategy: Plan how to improve your global health program using knowledge management interventions.
- Create and iterate: Use new knowledge management tools and techniques or adapt existing ones to meet your global health program’s needs.
- Mobilize and monitor: Implement knowledge management tools and techniques, monitor their effects, and adapt your approaches and activities to respond to changing needs and realities.
- Evaluate and evolve: Explain how well you achieved your knowledge management objectives, identify factors that contributed to or hindered your success, and use these findings to influence future programming.
Many of us practice knowledge management every day without realizing it. When health care providers refer to the latest guidelines on how to treat a disease, they are using knowledge management. When a program manager rolls out a new mobile application to facilitate communication between community health workers and their supervisors, they are all using knowledge management.
What do these approaches and activities have in common? They help global health practitioners share and apply valuable know-how in their work. The results? A stronger health workforce, better health services, and longer, healthier lives.
Summary/Key Messages
Knowledge is one of our most valuable assets to address global health challenges. What we know impacts what we do—and so how we manage knowledge can affect individuals, communities, and, ultimately, the health, social, and economic status of the world.
Global health organizations that adopt knowledge management strategies and practices can strengthen the performance of health care workers and programs. By doing so, they can improve health outcomes and even save lives.
Definitions
Data: raw building blocks of information (numbers, statistics, individual facts)
Information: data presented in a useful, structured, and meaningful way
Knowledge: the capacity to act effectively
Knowledge management: a systematic process of collecting and curating knowledge and connecting people to it so they can act effectively
Take a Course
The following three courses are part of the Organizational Change and Knowledge Management program. In our ever-changing and interconnected world, public health organizations, program managers, and health care workers need to be agile in their ability to constantly acquire, change, and adapt their practices based on the latest life-saving evidence. Adopting change management and knowledge management strategies and practices can strengthen the performance of health care workers and programs.
- Data Visualization—An Introduction:
In this course, participants will learn to identify their audience; find a story in a set of data appropriate for a target audience; understand the process of developing simple but compelling data visualizations; share and disseminate the visualization; and promote ongoing use of the data to inform decision-making. - Knowledge Management in Global Health Programs:
This course provides a basic understanding of why knowledge management is important to global health. Learners will gain techniques for getting essential, evidence-based knowledge into policy and practice. - Online Communities of Practice for Global Health:
Online communities of practice are increasingly popular vehicles for capturing knowledge, managing information effectively, collaborating virtually, and improving access to and quality of health services with limited resources. This course provides key considerations and strategies for building, nurturing, and monitoring these communities.
Other relevant courses include:
- Social Media for Health and Development:
Social media gives users the ability to reach a large audience over a large geographic area, offering great potential for social knowledge management. This course will walk the user through ways to share information through multiple channels in order to easily engage broad audiences on a global scale. - Journal Manuscript Development for Global Health:
Global health professionals are continually gathering valuable research and programmatic experience. Publication of this knowledge in peer-reviewed journals is a key knowledge management activity. This course will offer learners advice on each step in the journal manuscript development process, from planning and preparation through submission of a final manuscript.
Review the Evidence
Limaye R, Sullivan T, Dalessandro S, Hendrix-Jenkins A. Looking Through a Social Lens: Conceptualising Social Aspects of Knowledge Management for Global Health Practitioners. Journal of Public Health Research 2017; 6:761. The authors discuss the evolution of knowledge management, then propose a conceptualization of knowledge management that incorporates human and social factors for use within a global health context. Their conceptualization of social knowledge management recognizes the importance of social capital, social learning, social software and platforms, and social networks, all within the context of a larger social system and driven by social benefit. They then outline the limitations and discuss future directions of our conceptualization, and suggest how this new conceptualization is essential for any global health practitioner in the business of managing knowledge.
Evidence-based programs, yes—but what about more program-based evidence? Glob Health Sci Pract. 2018;6(2):247-248. Policy makers and program managers are better enabled to draw relevant lessons from implementation research and program experience elsewhere when there is richer documentation on what was done and what key contextual factors may have influenced outcomes. Newly developed Program Reporting Standards from WHO provide helpful guidance on what is needed for optimally useful documentation.
Coffey PS, Hodgins S, Bishop A. Effective collaboration for scaling up health technologies: a case study of the chlorhexidine for umbilical cord care experience. Glob Health Sci Pract. 2018;6(1):178-191. Facilitating factors for the
Chlorhexidine Working Group: (1) strong, transparent leadership by a neutral broker, promoting shared ownership among all members; (2) reliable internal and external communication; (3) well-defined terms of reference building on common interest around a simple, effective health intervention; (4) clear benefits of participation, including access to evidence and technical assistance; and (5) adequate resources to support the secretariat functions.
Koek I, Monclair M, Anastasi E, ten Hoope-Bender P, Higgs E, Obregon R. Doing what we do, better: improving our work through systematic program reporting. Glob Health Sci Pract. 2018;6(2):257-259. WHO has recently published program reporting standards to guide the type of information that reproductive, maternal, newborn, child, and related health programs should document to promote cross-program learning. The authors strongly encourage partners and key stakeholders to make use of the new standards as part of their routine program reporting.
Mugore S, Mwanja M, Mmari V, Kalula A. Adaptation of the training resource package to strengthen preservice family
planning training for nurses and midwives in Tanzania and Uganda. Glob Health Sci Pract. 2018;6(3):584-593. Lessons learned when adapting the evidence-based global family planning training resource package included the need to: (1) engage key nursing and midwifery educators for buy-in; (2) update the technical skills of educators in contraceptive
technology and competency-based training methods; and (3) adapt to the local context including condensing the global content for the time-limited pre-service education context.