Postpartum and Post-Abortion Family Planning Indicators: Learnings from Nigeria, Burkina Faso, and Rwanda

On August 17, Knowledge SUCCESS and the FP2030 NWCA Hub hosted a webinar on postpartum and post-abortion family planning (PPFP/PAFP) indicators that promoted recommended indicators and highlighted successful implementation stories from experts in Rwanda, Nigeria and Burkina Faso.
- Moderator:
- Alain Damiba, USAID WCARO
- Panelists:
- Yusuf Nuhu, FP2030 NWCA Hub
- Marie Claire Iryanyawera, UNFPA Rwanda presented on behalf of Dr. Francois Regis Cyiza, Rwanda Biomedical Centre, MOH
- Dr. Olufunke Fasawe, CHAI Nigeria
- Cheick Ouedraogo, Jhpiego Burkina Faso
Below we’ve included a comprehensive recap that links to exact segments within the full recordings (available in English and French). Click here to read the post in French.
Context And Background
Alain Damiba provided background about the work that was started back in 2017 by the measurement subcommittee of the FP2030 Postpartum and Post-abortion Global Steering Committee. Following a series of consultations, recommended indicators were developed which were then included in the High Impact Practices.
Watch now: [1:49]

Despite progress made, Alain discussed challenges that remain today in progressing toward global goals, including weak health systems, difficulties setting up Health Management Information Systems (HMIS) policies and processes, and implementation hurdles. There are opportunities thanks to universal health coverage policies being developed and free family planning, increases in Antenatal care (ANC) visits and in-facility deliveries and expansion of community approaches.
Reviewing The Indicators
Yusuf Nuhu presented the indicators that were developed and recommended for routine collection in national HMIS.
Watch now: [6:58]

These indicators help to ensure quality of services and access. Integrating these indicators into health systems will contribute to better decision-making for programs as countries accelerate towards their family planning goals.
Rwanda’s Experience
Marie Claire Iryanyawera, UNFPA Rwanda presented on behalf of Dr. Francois Regis CYIZA Rwanda Biomedical Centre, MOH, who was then able to join and contribute to the Q&A portion of this webinar.
Marie Claire gave an overview of the Rwanda context and their journey in introducing the indicators into their HMIS. Following a pilot of postpartum IUD in 2011-2014, Rwanda was ready to implement the new WHO Medical Eligibility Criteria (MEC) when it was released in 2015. Rwanda prioritized aligning their family planning training manuals with the revised MEC.
Watch now: [14:05]
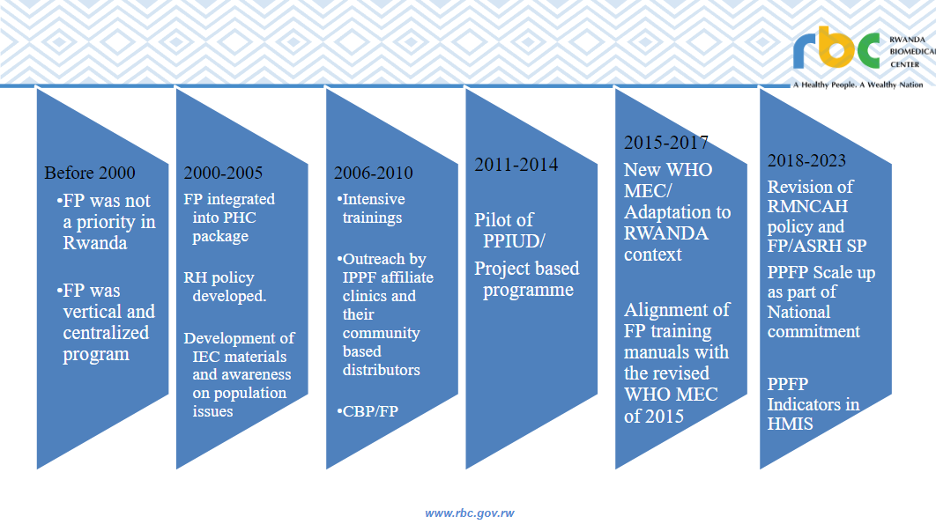
This timeline shows key policy milestones that contributed to an enabling environment for Rwanda to advance access to quality PPFP services.
PPFP is now scaled up in all health facilities nationally. Track 20’s FP Goals analysis for Rwanda, conducted in 2018, showed the potential to increase modern contraceptive prevalence rates (mCPR) by 3.8% per year if recommended family planning interventions were scaled up, with PPFP making up 19% of the scale-up program.
Rwanda defines postpartum period as one year post delivery. The adoption of the PPFP before discharge indicator was prompted by the significant number of women receiving antenatal care and high rate of deliveries at health facilities.
Nigeria’s Experience
Dr. Olufunke Fasawe shared CHAI Nigeria’s experience supporting the Federal Ministry of Health in integrating postpartum family planning indicators into the national health management information system (HMIS) in Nigeria.
The program Dr. Fasawe is sharing was conducted between 2016-2019 in Katsina, Kano and Kaduna states in northwestern Nigeria. Home delivery rates were very high at the time in these states, on average 80% and up to 91% in Katsina. The objective of the project was to train healthcare workers to insert Immediate Postpartum (IPP) IUDs and implants and reaching women during antenatal care to retain them to deliver in the facility where they could have access to immediate PPFP care. The project also focused on Traditional Birth Attendants who typically accompany home births and are in a position to refer women to a facility within 48 hours to receive PPFP. The project purposefully used this opportunity to build on previous CHAI work to strengthen the referral transport system using motorbikes.
Over the three year period, the project achieved good results in terms of uptake of implants and insertions within 48 hours after delivery whether the woman delivered in a facility or at home.
The registers are usually reviewed and updated every three years and the timing was good when indicators were recommended. Together with key partners they successfully incorporated three indicators measuring IPPFP, ANC and counseling into FP, labor & delivery and ANC registers. Dr. Fasawe shared screen shots from the registers themselves and the DHIS2 indicators. These indicators are now routinely reported and the Federal Ministry of Health is still prioritizing capacity strengthening on reporting and improving data quality.
Watch now: [37:20]
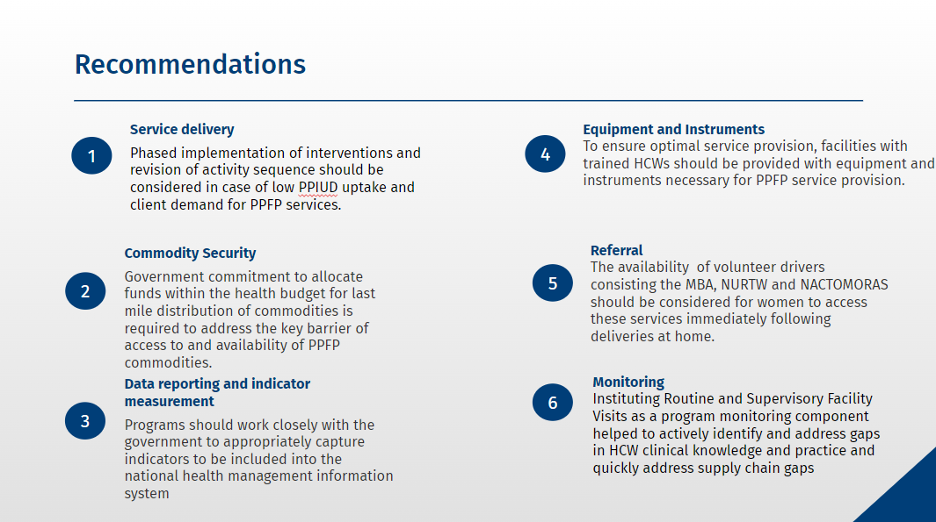

Dr. Fasawe shared six actionable recommendations related to service delivery, commodity security, data reporting and indicator measurement, equipment and instruments, referral and monitoring.
Burkina Faso’s Experience
Dr. Cheick Ouedraogo presented about Burkina Faso’s experience adopting PPFP and PAFP indicators into their HMIS. The data collection tools were reviewed and revised to account for new data needs, including FP, L&D, counseling registers and the monthly activity report template. Dr. Ouedraogo shared the multi-step methodology undertaken by Jhpiego and key stakeholders in Burkina Faso, including training managers and healthcare providers. A Steering Committee led this collaborative process.
Watch now: [52:04]

Three IPPFP and PAFP indicators were included in Burkina Faso’s national HMIS.
Dr. Ouedraogo shared the challenges encountered, in particular around data quality, ensuring providers were trained to collect this data, and shared perspectives for others to consider.
Q&A
Watch now: [1:09:31]
Marie Claire, what is the ratio of facility-based delivery to home delivery in Rwanda?
Answer: The latest Rwanda DHS of 2020 indicates that 94% of deliveries are assisted by a skilled provider.
Marie Claire, it's impressive to see the rapid increase in uptake of PPFP in such a short period of time. It is also a very rapid increase. Have there been any concerns raised about ensuring voluntary use (or non use)? Curious too if the government has invested in any data collection efforts to look at quality of care, method satisfaction, and discontinuation rates.
Answer: All health care providers are trained on PPFP counseling to ensure human rights based principles. It is voluntary, and data collection from ANC and in maternity services enable the collection of information. In addition, every two years, UNFPA supports the Service Delivery survey and client satisfaction counseling before the method and HRBA are part of the collected variables.
Dr. Cheick, I'd like to better understand the specific process you followed to include the post-abortion family planning indicators in the National Health Information System and how it may have differed from the process of including the postpartum family planning indicators.
Answer: The same process was used as for the PPFP. For the PAFP, we strengthened providers’ skills in exploring values and transforming their attitude towards PAC, despite the fact that it is part of the minimum service package for their level of care. This helped to dispel fear and stigmatization.
Dr. Cheick, the training was for providers but what if the community is not ready—what can be done for the community?
Answer: The demand generation was undertaken by Community Health Workers. In addition we have organized dialogues with community leaders on sexual and reproductive health and rights which helped to motivate the community to accept FP services.
Dr. Cheick, please explain the strategies used to increase from 1% to 43%.
Answer: Due to stigmatization and discrimination, even when the service has been provided they did not record it. As such, we have organized values clarification and attitude transformation, which reinforce their confidence and beliefs. A monthly monitoring of data and supportive supervision put in place contributed to an increase in the uptake of PAFP. The last one was the placement of commodities in the procedure room.





