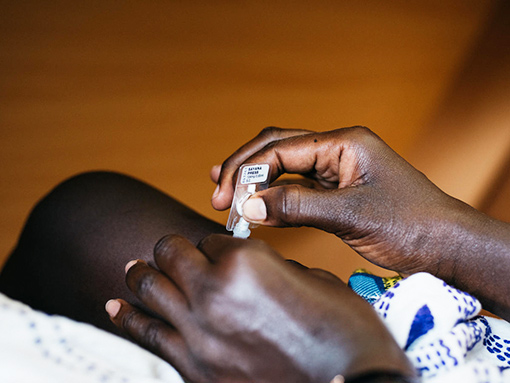
How can the health system attain data on self-care (e.g. uptake, perceptions, and attitudes, etc.)? How can self-care be measured?
Professor Fredrick Makumbi: Data on self-care can be attained through village health teams, which should be trained to ensure that data is collected correctly. Other sources for self-care data may include drug shops, which should similarly be trained, empowered, and supported to generate such data; local and national level surveys; and monitoring of the HMIS on family planning services.
What are some of the benefits (to individuals and health systems) of advancing self-care for SRHR?
Dr. Olive Sentumbwe, the Family Health and Population Officer at the World Health Organization (WHO) Country Office in Uganda: Self-care interventions offer a strategy to reach people with quality health care services and information. They enable individuals to access and utilize SRHR information and services without discrimination or experiencing stigma. In addition, self-care increases confidentiality, eliminates barriers to access, improves individuals’ autonomy, and enables them to make decisions regarding their own health without feeling pressured, especially among vulnerable populations like the young people. For some individuals, self-care is acceptable as it preserves their privacy and confidentiality and removes bias and stigma which may result from providers during times of client-provider interaction. In the long run, once the individual beneficiary learns where to get the product and how to use it effectively, it becomes cheaper and under the control of the user. Self-care will bring improved mental well-being and increase agency and autonomy particularly for the vulnerable groups. Research suggests that self-care promotes positive health outcomes, such as fostering resilience, living longer, and becoming better equipped to manage stress.
Self-care eases the stretch on the health system and enhances efficiencies in handling critical health issues. For instance, the management of the COVID-19 pandemic resulted in the reassignment of a significant portion of health providers to COVID-19 case management, hence reducing the bandwidth of skilled human resource available to respond to the non-COVID-19-related health needs of individuals. Self-care increases coverage of some services to the public, however, when self-care is not a positive choice but born out of fear or because there is no alternative, it can increase vulnerabilities and lead to poor health outcomes.
How can self-care for SRHR facilitate the advancement of the gender equality and equity agenda in Uganda and enable women to exercise their health rights?
Ms. Fatia Kiyange, deputy executive director at Center for Health Human Rights and Development: Self-care interventions for SRHR unleash power into the hands of women and girls. This allows them to take care of their own health, giving them choice and autonomy.
Women and girls grapple with a range of SRHR-related issues, ranging from the inability to access and utilize modern methods of contraception to preventing sexually transmitted infections and reproductive-health cancers.
As such, self-care becomes a reliable and effective approach for responding to the SRHR needs of women and girls in the most affordable, confidential, and effective manner while maintaining quality of care.
What challenges/lessons/best practices have you observed in the process of advancing self-care interventions at the national level, using DMPA-SC as an example?
Ms. Fiona Walugembe, project director at Advancing Contraceptives Options, PATH Uganda: Disposal of used injectables, integration of data on self-care into the Health Management Information System (HMIS), inadequate time for health providers to effectively train users in self-injection, stakeholder buy-in for self-care and lengthy policy approval processes were the most outstanding challenges encountered as we scaled up the DMPA-SC in Uganda.
Dr. Lillian Sekabembe: Potential product stock-out due to interruptions in the supply chain and the health system’s readiness to entrust individuals with information and products have been key challenges that affect advancing self-care.
Ms. Fiona Walugembe: Whereas self-care has been in existence, its use in the SRHR realm is relatively new. Stakeholders need to think creatively, use evidence, and collaborate with experts as well as influential leaders in championing the concept. Best practices, such as the use of human-centered design approaches for program design, establishing monitoring and evaluation frameworks as well as leveraging existing health systems are critical.
What can be done to ensure that self-care does not become “a poor man’s” solution to the problems of the health system?
Dr. Moses Muwonge: Self-care for SRHR will be implemented in the public sector where free services are [already] provided. This will include community health workers who will reach out to vulnerable communities and build their self-care awareness. While on the other hand, the expectation is that those who can afford it will access products for self-care from the private sector, where individuals buy commodities and services they need.
What’s the vision for success for self-care in Uganda?
Dr. Dinah Nakiganda: At the start of the process, stakeholders struggled with developing a vision for structuring self-care in Uganda. However, through the SCEG, stakeholders hope to see an increase in awareness of the self-care concept, community acceptance of self-care, and integration of self-care interventions with respect to governance in order to strengthen health systems and achieve universal health care coverage.