Did You Miss FP2020’s Webinar on “Exploring Digital Platforms for Family Planning During COVID-19”?
Here’s What You Need to Know.

FP2020’s webinar on digital health for family planning during the COVID-19 pandemic brought together presenters from a variety of projects, all of which are leveraging technology to meet the needs of their clients in new ways. Missed the webinar? Our recap is below, and so are links to watch for yourself.
Digital health solutions and platforms—from telehealth to client-centered apps to data management systems—can empower patients and help ensure continuity of voluntary family planning. In the COVID-19 era, these solutions are even more critical as communities face lockdowns and a shortage of family planning supplies.
As Martyn Smith, FP2020’s Managing Director, remarked in his introduction to the Exploring Digital Platforms for Family Planning During COVID-19 webinar on June 16, we are witnessing the “rapid transformation and potential of technology as a critical healthcare tool.” Presenters in the webinar expanded on the many benefits and opportunities digital health solutions can provide as we address the challenges of COVID-19, particularly for family planning and reproductive health.
Weren’t able to catch the webinar live? No problem! Keep reading for highlights from each presentation, or watch the full webinar recording in English or French.
Introduction to Digital Health (07:20 – 19:00)
Trinity Zan, Associate Director, Research Utilization, Research Utilization Lead, Research for Scalable Solutions Project, FHI 360
Definition of digital health (sometimes referred to as “mHealth” or “eHealth”): The field of knowledge & practices associated with the use of development and use of digital technologies to improve health (WHO “Global Strategy on Digital Health”).
What digital health looks like: Digital health can help us with a number of functions that can improve service delivery, research, and other efforts—from making and receiving voice calls and SMS messages to providing job aids and managing health data. We can also use various channels to implement digital health—including apps, websites, and social media. Some digital health tools serve providers (for example, online counseling tools), others focus on clients (for example, personal health apps/trackers), and still others focus on supporting systems (for example, an Electronic Medical Register). Digital interventions can also overlap and serve multiple groups—for example, telehealth, which is an interaction between a provider and a client.
What we know about digital health for family planning: Digital interventions can support a change in knowledge and attitudes about family planning, and are particularly attractive to young people. Evidence shows increased efficiency and accuracy with digital systems like registers and data collection systems. While we have an increasing evidence base related to how these digital tools can improve provider knowledge and competency using digital tools, we have limited and mixed evidence about the impact of digital health on behavior change and cost-effectiveness of digital health interventions.
More information on digital health for family planning:
- The WHO has helpful general tools for digital health (WHO’s Recommendations on Digital Interventions for Health Systems Strengthening, WHO’s Classification of Digital Health Interventions, The MAPS Toolkit).
- For implementation considerations, see Principles for Digital Development.
- Specific to Family Planning, there are two High-Impact Practice (HIP) briefs—Digital Health for Social and Behavior Change and Digital Health for Systems—to help us understand the evidence and implementation guidance for digital health.
Sehat Kahani (19:00 – 32:45)
Dr. Sara Saeed Khurram, Co-Founder and CEO, Sehat Kahani (Health Story), Pakistan
What Sehat Kahani does: There is an overall shortage of doctors in Pakistan. At the same time, many female doctors stop practicing after getting married. Sehat Kahani was founded to address these issues by providing telemedicine solutions to patients in need, using a pool of online female doctors.
They have two main interventions:
- Telemedicine clinics
- A health-based mobile application.
Patients can walk into a Sehat Kahani clinic, consult with a physician (via telehealth) and a nurse (in person), and then obtain the services and referrals they need. They also have access to a medical helpline (open 24 hours a day and 7 days a week). The graphics below show a patient’s journey through a Sehat Kahani clinic and the mobile app.
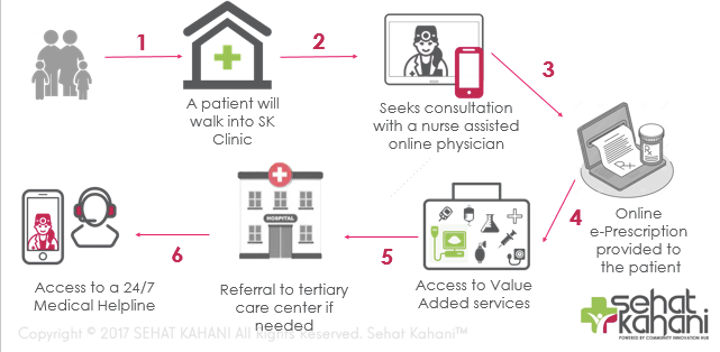
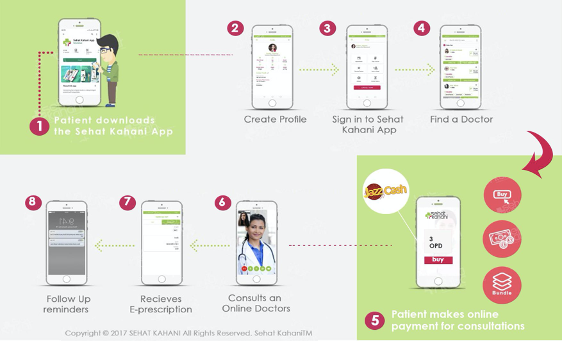
Impact of their work: To date, this program has resulted in 165,000 eHealth consultations in 26 eHealth clinics. Most of these consultations are for women and children, and about 20% have involved family planning and reproductive health. The app has reached over a million people, and there have been more than 25,000 consultations. Sehat Kahani has extensive community outreach in remote areas, and uses real-time data analytics to identify and address disease patterns.
How Sehat Kahani is responding to COVID-19: Sehat Kahani provides telemedicine platforms to women in Pakistan who are not able to access family planning during the COVID-19 pandemic, and to provide medical services to COVID-19 positive patients in their own homes. They have also partnered with the Government of Pakistan to make the app available for all, in response to COVID-19.
Honey & Banana (32:45 – 46:40)
Ms. Maja Kehinde, DKT Nigeria, Manager, Honey & Banana, Nigeria; Nirdesh Tuladhar, Marketing Director at DKT International, Nigeria
What Honey & Banana does: A digital initiative of DKT Nigeria, Honey & Banana features blogs, quizzes, and stories on family planning topics. It includes youth-friendly messaging to educate and entertain users. A live chat feature connects youth and medical experts to help answer their questions about contraception. There is also a referral feature, where followers are linked to DKT partner clinics to obtain their chosen method of contraception. Finally, they manage a toll-free call center that provides information and referrals for offline users.
How Honey & Banana is responding to COVID-19: Starting in February 2020, the program updated their call scripts and messaging — for example, mentioning contraception as an essential service needed during the COVID-19 lockdown. The call center also provided waiver letters for referred clients, so clients could access clinics without being harassed by checkpoints during lockdown. Website stats peaked in April after the lockdown began — with over 17,000 website visits compared with about 7,400 the previous month. Social media engagements also increased around that time, and referral services increased. Use of the digital platform during the COVID-19 era shows an increase in questions from men asking about contraception. The questions also have skewed more towards emergency contraceptive methods, missed pills, and pregnancy prevention.

Recommendations for other digital platforms:
- Understand the target audience, their behavior, and their lifestyle.
- Build a strong brand—visibility and credibility increases use of digital platforms.
- Establish a robust referral system, and establish strong, ongoing partnerships with clinics.
Nivi (46:40 – 1:00:00)
Ben Bellows, Co-Founder and CBO, Nivi
What Nivi does: Nivi is a consumer-facing digital health company. They engage consumers in a variety of countries—including Kenya, India, and South Africa—to help them access information and catalyze behavior change through popular messaging platforms (for example, WhatsApp). They also serve and support family planning programs, producing insights for partners about user engagement.
How Nivi is responding to COVID-19: With the onset of COVID-19, Nivi created COVID-19-specific conversations to address challenges in accessing family planning and reproductive health care. From April 7-May 11, they reached 12.6 million people through targeted messaging, and engaged 93,682 Nivi users in 185,000 conversations about family planning and COVID-19. The platform started inferring and predicting information their users might need, based on their responses or requests. See the photos below for examples of these conversations.
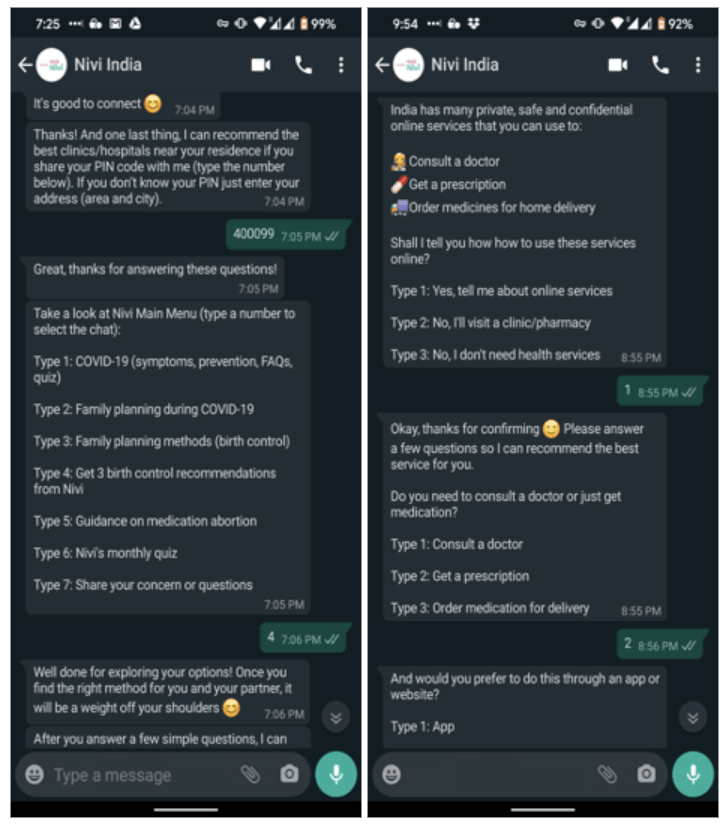
According to the data obtained during these conversations, Nivi identified barriers to obtaining family planning during COVID-19. For example, when asked “What was your experience seeking family planning at the pharmacy within the past month?”—half of users reported that they did not get the information they intended to get, due to stockouts or closed pharmacies. The majority of users also responded “yes” to the question “Would you like to know about online services?” In response to these insights, and in collaboration with partners like PSI India, Nivi is now running integrated services with pharmacies. With six pharmacies, Nivi conducts online sessions and asks users targeted questions to provide the best pharmacy options and services for them. This enables the users, who would otherwise face access barriers, to obtain family planning consultations and products. The objective of this initiative is to integrate virtual solutions into existing pharmacy programs—and to meet the challenges faced during the COVID-19 era.
Highlights from Question and Answer Session (1:00:00 – 1:30:00)
Participants asked a range of questions after the presentations, on topics from cost-effectiveness to reaching young people. Below is a summary of selected questions and answers (note that these are not actual transcriptions).
What evidence exists for the feasibility and effectiveness of e-Commerce platforms within family planning?
Trinity Zan: “This is a new area for family planning. There are multiple platforms working at the global level. Some groups are working to produce evidence, but we are still nascent enough that there isn’t much documentation.”
Ben Bellows: “For more of an integrated consumer experience, programs could incorporate a physical product but also a way to learn more about the product through messaging and support lines.”
Is there evidence on the scalability of digital health solutions for family planning that is adaptable for a country like Uganda?
Trinity Zan: “There are multiple services that have scaled up—for example, FHI 360’s Mobile 4 Reproductive Health (m4RH) initiative was scaled up widely. A number of resources (including the HIP briefs and the MAPS Toolkit) offer information and evidence on scale up.”
Is there any evidence on the equity of the impact that Sehat Kahani is having?
Dr. Sara Saeed Khurram: Low-income communities often lack access to health services, and have to travel to obtain services. However, across income brackets, there are issues with quality, accessibility, and affordability of healthcare. And even when doctors are available, often men in families will obtain services before women.
What challenges have you seen in terms of young people and adolescents accessing digital platforms?
Dr. Sara Saeed Khurram: “One challenge is adapting to virtual doctors as opposed to physical doctors’ visits. There are also issues with digital payments. Also, young people sometimes have issues accessing mobile devices and getting to physical clinics. However, once they access the services, young people have had a great response to the Sehat Kahani program.”
Trinity Zan: “While there are challenges in young peoples’ access to digital platforms, there are also opportunities, since young people have an interest and willingness to use these platforms. It is important for us to co-design these platforms with young people, to mitigate these barriers.”
Nivi is a great platform, but how would this work for women in India who don’t have a phone or don’t speak English?
Ben Bellows: “There are 400 million Facebook users in India alone. Close to one billion individuals between the ages of 15-35 have a phone line (a SIM or data access point) in low- and middle-income countries. While there are challenges accessing phones, there are opportunities as more young people are online. We anticipate even more users as costs go down and access improves. 80% of Nivi users in India access their conversations in Hindi—we are also adding more languages. In Kenya, about half of users access content in Swahili. In South Africa, they are operating in English and adding languages over time.”
Is there a need for a large backroom operation to keep these platforms going and ensure they’re operational?
Dr. Sara Saeed Khurram: “You don’t need more resources, but you need more efficiency. Important to automate systems to take the workload, so you don’t need as many people on the backend. This will help provide access to a lot more people in a lot more countries.”
Ms. Maja Kehinde: “Basically you just need individuals to manage communication, messaging, and answer questions. You can often start with two individuals at first.”
Is the digital approach a cost-effective way of reaching the poorest women of reproductive age and getting family planning to them?
Dr. Sara Saeed Khurram: “There is a huge stigma around family planning in Pakistan. Women generally don’t reach out to health workers because of a lack of knowledge of family planning. Providing mobile services can help bridge this gap.”
Ben Bellows: “Think big and act big. With a larger number of users, this becomes very cost-effective. We can look at behavior and infer information about users to determine if we are reaching the poorest populations. We can also ask users what they prefer and co-create platforms with users.”
Trinity Zan: “It depends on the type of service that you’re offering. This can mean different preferences, fixed costs, and ongoing costs. It is hard to make blanket statements about resources required since there is a lot of diversity in platforms and initiatives. Also, within family planning, we don’t have a lot of data about what is needed to reach the most marginalized. We do know that sometimes the costs to reach the most marginalized are higher. There is potential for these platforms to be cost-effective, but we need more information about the status quo services as well as the cost to run these digital interventions.”




