Scaling up Contraceptive Implants: Case Closed or Untapped Potential?
The introduction and scale-up of contraceptive implants have unequivocally increased access to family planning (FP) method choice around the world. Late last year, Jhpiego and Impact for Health (IHI) collaborated to document the experience of contraceptive implant introduction over the last decade (primarily through a desk review and key informant interviews) and identified recommendations to scale up implants in the private sector. This piece summarizes some of the key findings available in the suite of resources available here.
Case closed or untapped potential? A debate
It is just over a decade since world leaders gathered at the 2012 London Summit on Family Planning (FP) and committed to one goal: meeting women’s unmet need for contraception. This goal was operationalized through the creation of Family Planning 2020 (FP2020), a global partnership to empower women and girls by investing in rights-based FP, and extended through FP2030 to reaffirm this global commitment. The emergence of FP2020 also paved the way for the introduction of the Implants Access Program (IAP) in 2013: a public-private partnership to increase access to contraceptive implants for women in low-income countries. The results are awe-inspiring: the IAP led to a 50% price reduction for those procuring implants for FP2020 countries and, over the past decade, annual global procurement of implants for FP2020 countries increased from 3.9 million to 10.6 million and is projected to increase further in the coming years. Implants have also been incorporated into national universal health coverage (UHC) plans, such as those in Ghana and Zambia. Further, an analysis considering recent and longer-term changes found that increases in implant use during this period were the main driver of mCPR gains in 11 countries in Africa. The introduction and scale-up of contraceptive implants have unequivocally increased access to family planning (FP) method choice around the world.
Does this mean we can close the book on implants, considering them fully mainstreamed? Or are there untapped frontiers for expanding method choice – choice that includes implants?
What made implants such a success story?
From our analysis (including a desk review and key informant interviews), meeting demand through implants is underpinned by a few key lessons.
- Coordinated action at all levels helped to fast-track implant introduction and scale-up; including national government stewardship and global coordination for investment, volume guarantees, clinical guidance, and sharing lessons learned.
- Ensuring availability of implants through multiple public service delivery channels (e.g. CHWs and mobile clinics in addition to primary healthcare centers) and task sharing were key strategies to increase access and uptake.
- Demand generation activities designed with providers and users helped ensure women could make an informed choice about contraceptive use and method choice, while also increasing acceptability of implants.
- Comprehensive quality assurance systems and training programs helped ensure quality of implant services – both insertions and removals – by a range of providers.
- Addressing price barriers through volume guarantees was critical for equitable access, but scale-up through the private sector will require new, innovative solutions and financing.
For the FP2030 goal to be realized, contraceptive implant availability, acceptability, accessibility and quality need to be maximized; however, a number of challenges remain.
An unfinished agenda?
Expanding method choice is an integral component of family planning programs. Some estimates indicate that for each new contraceptive method added to the mix/basket of choice, overall contraceptive prevalence in a country will rise 4-8%. But sustaining such expanded choice over the long term requires attention to method-contextual delivery features – features that, if ignored, could stifle a method’s ability to meet the needs of individuals and couples who wish to use it. For contraceptive implants, such features requiring continued attention include:
Removal access: Improving access to quality implant removal helps to meet clients’ rights, helping ensure that they have full, free, and informed choice to both use and stop using their method. However, data continue to demonstrate a disconnect in access and utilization of quality implant removal services when compared to implant insertion. A recent study using Performance Monitoring for Action (PMA) service delivery point data in 6 countries in sub-Saharan Africa indicates that a substantial proportion (31-58%) of implant-providing facilities report at least one barrier to offering implant removal services.
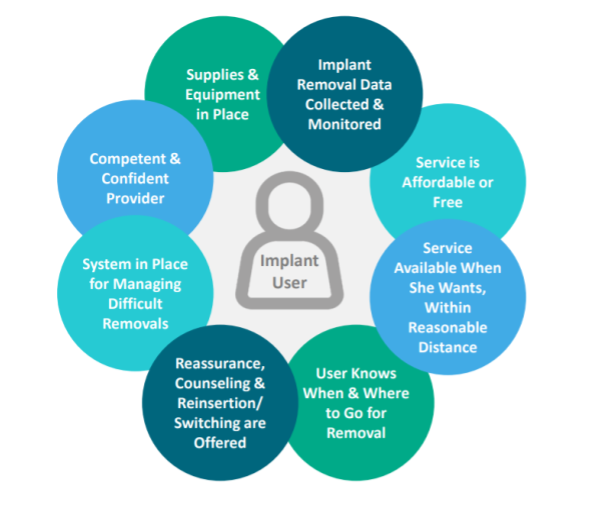
Developed by the Implant Removal Task Force, these eight standards need to be upheld to satisfy clients’ implant removal needs (further questions program managers can explore to ensure removal-inclusiveness are included here):
- Providers are competent and confident. Are continuing education, refreshers, and recertification opportunities offered for healthcare workers providing implant services to ensure that their skills are up to date?
- Adequate supplies and equipment are in place: Are adequate equipment and consumable supplies in place for both standard and difficult implant removals at service delivery points?
- There’s a system in place for managing difficult removals: Is there adequate coverage of healthcare workers who can localize and remove non-palpable implants?
- Implant removal data is collected and monitored: Are systems in place to collect and use HMIS data to understand coverage, source, utilization, and outcome of implant removal services?
- Implant removal services are affordable (or free): Is the cost of removal equal to or less than the cost of insertion, and are financial mechanisms in place for clients who cannot pay?
- Implant removal services are available when the user wants, and within reasonable distance: Are all facilities that offer implant insertions able to offer implant removal services? And when not, are referral mechanisms in place?
- The implant user knows when and where they can go for removal: Do healthcare workers provide accurate communication about when, where, and why removal services can be accessed?
- At the time of removal, reassurance, counseling and reinsertion or method switching are offered: Do service delivery sites offering implant removal services have a full range of FP method choices for clients who desire implant reinsertion or a different method of choice?
A suite of materials to support program managers, technical advisors, and other FP program stakeholders in designing, implementing, and measuring FP programs with an implant removal-inclusive lens is available here.
Private Sector Expansion: The last decade is testimony to how coordinated efforts have transformed women’s access to implants in the public sector. A recent analysis of 36 countries showed that 86% of implant users obtained their implant from a public-sector source. To maximize the private sector’s ability to deliver implants, a similarly coordinated effort, led by national governments and global partners, can release the untapped potential of the private sector to deliver contraceptive implants at greater magnitude and contribute to FP2030 goals. Such efforts should focus on transforming four key areas:
- Supply: Currently, the implant supply chain and market are reliant on donor funding, which negatively impacts long-term sustainability. This severely curtails private sector healthcare outlets’ interest and ability to access affordable contraceptive implant commodities – and suppresses any business case to do so.
- Training: Historically, opportunities for implant training have not met private providers’ needs, resulting in a lack of insertion and removal skills and quality assurance measures. This, in turn, hinders quality-assured service delivery. Training that meets the needs of private providers can transform their ability to provide quality implant services.
- Demand: With a free ‘supply’ of implants widely available in public sector facilities, a key challenge to creating demand for implants in the private sector, is elucidating why a woman should pay for this service. What additional benefits are gained by accessing this service in the private sector? And which of these benefits resonate most with the target consumer?
- Stewardship and Coordination: As the last decade demonstrated in the public sector, for change to occur, efforts need to be appropriately stewarded and carefully coordinated. National governments are best placed to steward these efforts in partnership with private sector actors who are represented by an appropriate private body to unify and represent the interests and voice of private sector providers.
What’s next? A call to action
In some ways this debate around contraceptive implants reinforces what we know about new method introduction and sustainable service delivery: the importance of considering mixed health systems actors (their opportunities, abilities and motivations) in new product introduction; using a rights-based lens to inform product introduction and service delivery in all contexts (e.g. not promoting one method over another) and so much more (this article doesn’t touch on the need to expand method choice in humanitarian contexts, for example!). But just because these principles are widely known doesn’t mean they’re easy to deliver.
This begs the question: is this a pivotal moment to reframe how we support implants to ensure sustainable choice and scale?
What could this look like in practice? We’d like to offer two concrete recommendations:
- Plan for service delivery through mixed health systems during (not after!) method introduction, paying particular attention to sustainable financing mechanisms (for supply and the service) and engage the private sector throughout the product introduction journey so they are motivated to deliver methods that are simultaneously subsidized in the public sector.
- Consider the full scope of a method’s use (including uptake as well as discontinuation or method switching) as a part of contraceptive method service and access. This is particularly important for implants, which require access to a service provider to discontinue the method (i.e. remove the implant). Planning for and supporting an individual’s choice to discontinue any contraceptive method is necessary to ensure autonomy, choice, and access to begin and end methods.
ABOUT: Jhpiego and Impact for Health, as a component of the Expanding Family Planning Choices (EFPC) project, undertook rapid literature reviews and key informant interviews with experts in the contraceptive implant and family planning field, to better understand programmatic learnings, tips, best practices and challenges, including the potential for private sector engagement for implant introduction and scale-up. The results of this review led to the development of a series of products for continued learning and sharing, available here.




